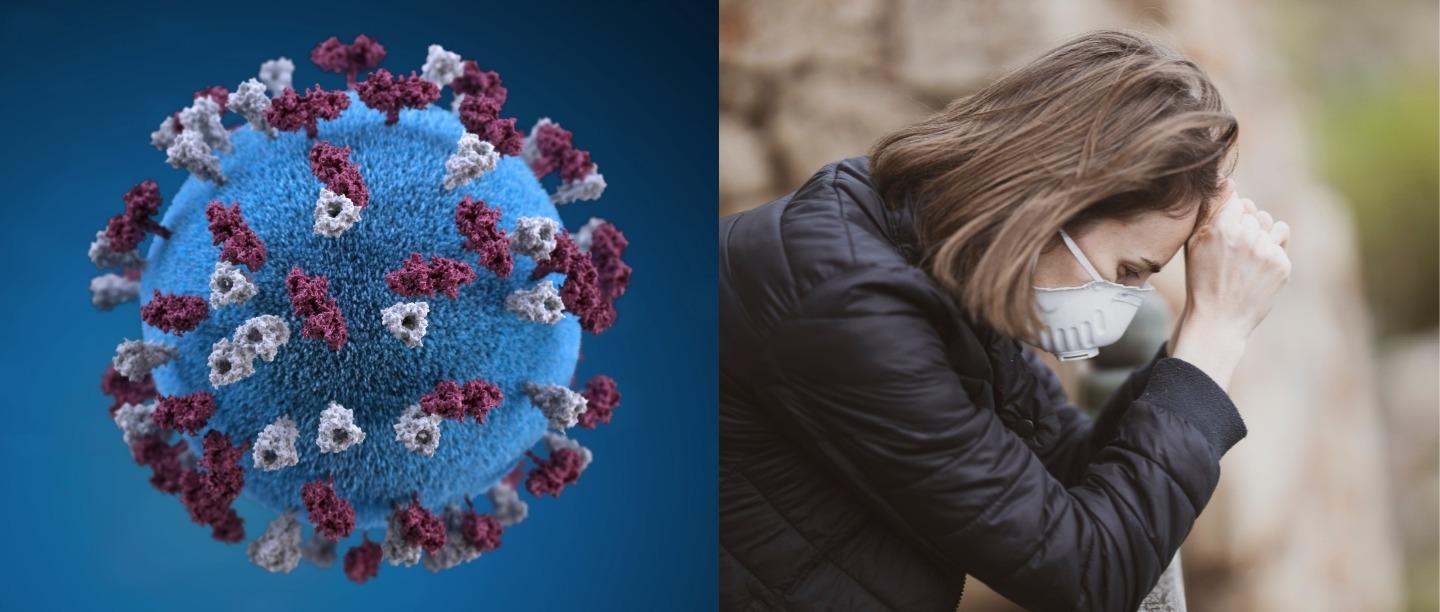
All the COVID-19 scares and the slew of pandemic news adding on to your stress levels? Well, we have bad news for you. According to a recent study, patients with high levels of the stress hormone cortisol in their blood are more likely to deteriorate quickly and die of COVID-19 than those with regular cortisol levels.
Cortisol is a hormone that is produced in the body to mediate stress response, regulate metabolism, and also the immune function of the body. The hormone is secreted in high quantities when we are presented by situations of stress. Thus a high level of this hormone mostly points at high level of stress or stress stimulants in the surrounding. When healthy & resting, our cortisol levels range from 100 to 200 nm/L approximately and tend to get nearly zero when we sleep. The levels also drop when we are severely ill and both severely high and low levels of cortisol can be dangerous for the patient.
The study, led by Indian origin Research Professor Waljit Dhillo and published in The Lancet Diabetes & Endocrinology on Thursday, provides the first data to demonstrate that cortisol levels are a marker of the severity of the COVID-19 infection. Simply put, those with higher levels of stress are relatively at a higher risk of catching a severe or life-threatening COVID-19 infection.
“From an endocrinologist’s perspective, it makes sense that those COVID-19 patients who are the sickest will have higher levels of cortisol, but these levels are worryingly high,” said professor Dhillo in a media statement.

The study has been funded by UK’s National Institute for Health Research (NIHR) and the Medical Research Council. It was conducted on 535 COVID-19 patients admitted to three London hospitals including Charing Cross, Hammersmith and St Mary’s. A COVID-19 swab test and routine blood tests including a baseline measurement of cortisol levels were conducted on these patients within 48hrs of their admission.
Besides, establishing cortisol as a marker for severe COVID-19 infections, the study also points at assessing cortisol levels to identify patients who are more likely to require intensive care when infected. As Professor Dhillo says, “Having an early indicator of which patients may deteriorate more quickly will help us with providing the best level of care as quickly as possible, as well as helping manage the pressure on the NHS. In addition, we can also take cortisol levels into account when we are working out how best to treat our patients.”
While the novel coronavirus has already infected more than 8 million people worldwide, hardly concrete information exists on its behaviour as well as aggravators. The study might prove to be a positive step in the right direction by throwing some light on how the coronavirus behaves for different patients.
Featured Image: Unsplash